Value-Based Care: What’s Not Working?
August 16, 2025
There is a widely held belief among healthcare experts that value-based care can reduce healthcare costs, improve healthcare coordination and quality of care, and help to alleviate physician burnout. Increasing evidence supports this belief.
That is why the Biden Administration aims to include all 34 million traditional Medicare beneficiaries in value-based arrangements by 2030, up significantly from 13 million in 2023. Similarly, Medicaid is embracing value-based care, with 41 states adopting capitated managed care. As of now, 72 percent of Medicaid beneficiaries are enrolled in comprehensive risk-based managed care organizations.
Nevertheless, administering value-based care arrangements is far from easy – and is critical to achieving the Quadruple Aim.
In our conversations with health plans, we hear six recurrent themes that highlight the challenges inherent to value-based care administration.
- “It’s hard to demonstrate near-term ROI, and even harder to forecast.”
A 2023 survey of 400 providers and payers showed more than a third (38 percent) of respondents believe the narrow definition of ROI significantly affects value-based care adoption. The study also found that 51 percent believe the requirement to prove near-term ROI is a significant factor in slowing the growth of value-based care. Only the reluctance to assume downside risk is believed to be a more significant factor than the requirement to prove near-term ROI.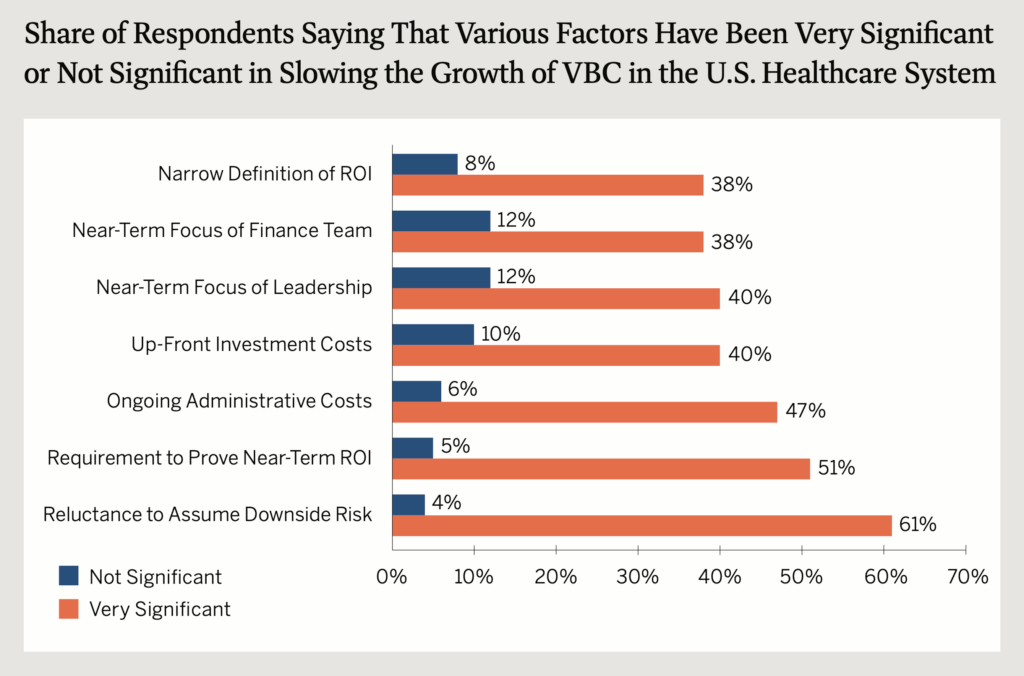 Source: 2023 Perspectives on Value-Based Care Survey Report
Source: 2023 Perspectives on Value-Based Care Survey Report - “We have no idea how we’re performing until the end-of-the-year settlement.”This is true for health plans and even more so for physician practices.The average US primary care practice reports 12 managed care contracts. Chances are that incentive programs and terms vary significantly between contracts, meaning it can be quite challenging for providers to know how to succeed in their value-based care arrangements.In fact, additional evidence from a 2024 Black Book Research survey suggests that providers do not inherently know how to succeed in value-based care. The survey found that two-thirds of healthcare providers in value-based care arrangements are “turning to advisory firms to navigate the complexities of addressing their challenges in care delivery, implementing effective data analytics strategies, and fostering collaboration among various stakeholders in the healthcare sector.”
- “Physicians are reluctant to join due to a perceived lack of transparency.”Data availability tops the list of capability gaps that have had a negative effect on the performance of value-based care programs, with 37 percent of respondents saying it has a major negative effect and another 37 percent saying it has a minor negative impact. Provider and payer survey respondents also cite gaps in analytic and IT/digital capabilities as negative impacts on value-based care performance.
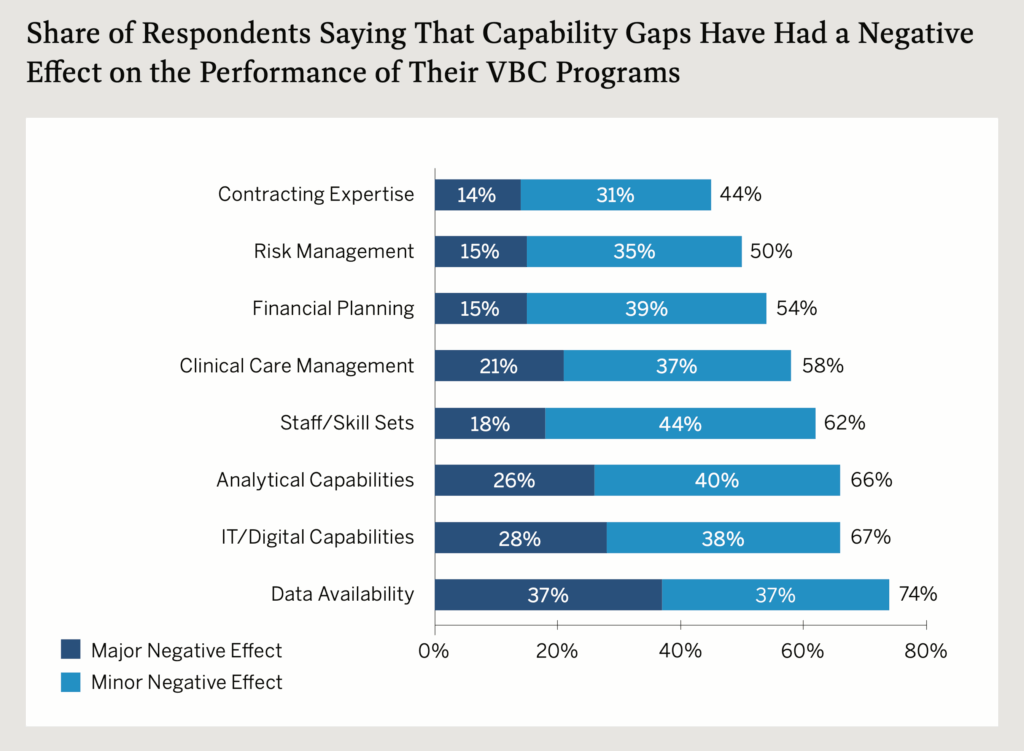 Chart Source: 2023 Perspectives on Value-Based Care Survey Report
Chart Source: 2023 Perspectives on Value-Based Care Survey Report - “Tracking performance requires a TON of manual Excel number crunching.”Health plans continue to increase the number of VBC contracts. One estimate suggests that statewide plans manage as many as 20 contracts, putting billions of dollars at risk. At the same time, too many plans are still managing these contracts with Excel spreadsheets, significantly limiting their ability to manage and impact performance.
- “Data is scattered across multiple systems – there is no one source of truth.”Many health plans have cobbled together multiple systems to administer their value-based care contracts, including a member attribution engine, member engagement platform, claims processing, provider performance reporting, value-based care contract builder and modeling platform, and more. This complicates health plans’ ability to administer value-based care contracts, and potentially more problematic, there is no single source of truth.
- “Quality metrics are great, but tracking is too slow for proactive engagement.”Ideally, health plans and their value-based care providers have near real-time, member-level data that identifies gaps in care such as mammograms and colonoscopies. Too many health plans are unable to attain and share this data in a timely manner that enables providers to close these gaps during the plan year. This hurts provider performance and also negatively impacts health plans’ Medicare Star ratings and efforts to attain/retain NCQA accreditation.
At NASCO, we believe that achieving excellence in value-based care requires embracing four key imperatives:
- A holistic approach
- Data transparency for health plans and providers
- Clarity about financial impacts
- Insight velocity
Stay tuned for a deep dive into the imperatives around which we are building and a guide to excelling at value-based care administration.
